CGM LYTEC is a trusted and affordable practice management solution that simplifies the way you run your practice.
With each release, CGM LYTEC gets better. Even more powerful. Every year, we add new layers of functionality and usability.
Discover some of the benefits of upgrading to CGM LYTEC 2026.

Why choose Dabbs Computer Consulting?
Dabbs Computer Consultants has over 20 years of experience helping small medical practices find the perfect medical billing platform. We understand that every practice is unique and has specific software needs. Whether you are a solo practitioner or have a team of over 20 providers, we can help you choose the software that best meets your needs.
Dabbs Computer Consultants doesn’t just sell software — we also provide training and support to ensure a smooth implementation. We know that switching to new software can be challenging, but our team is there to help you every step of the way.
We offer a variety of approaches to medical billing, so you don’t have to worry about being forced into an electronic health records (EHR) system if you’re not ready for it. Our goal is to find the best solution for your specific needs.
CGM LYTEC – Trusted and affordable medical billing software with new layers of functionality added every year.
eMEDIX Clearinghouse by CGM – Fully integrated with LYTEC 2026
Through eMEDIX, your practice management software and clearinghouse come together under one roof with CompuGroup Medical.
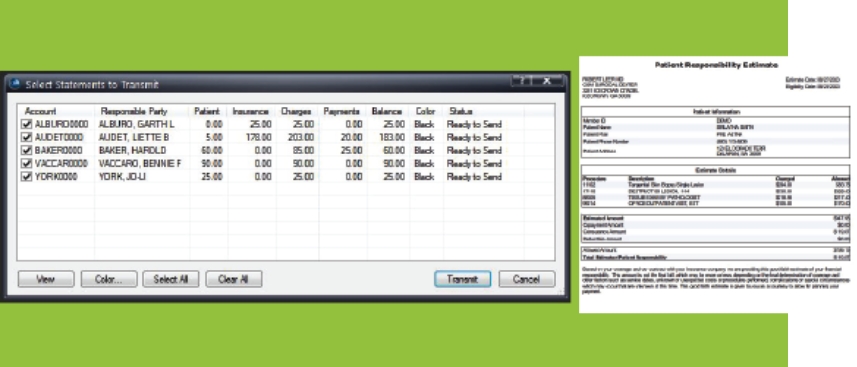
Patient statements are fully integrated with CGM LYTEC 2026 — no more logging in to third-party websites to view statements! Designed to be familiar and easy to use, providers can preview statements before transmission.
Review statements from within CGM LYTEC to answer any patient questions, and use eMEDIX to access reports, including statement confirmations and undeliverable or changed patient addresses. When you adopt the eMEDIX online payment portal, a QR code will appear on your statements to direct patients to the portal.
Combine your integrated patient statements with our industry-leading eMEDIX clearinghouse and consolidate your operations under one trusted vendor.
Why choose CGM LYTEC 2026 medical billing software?
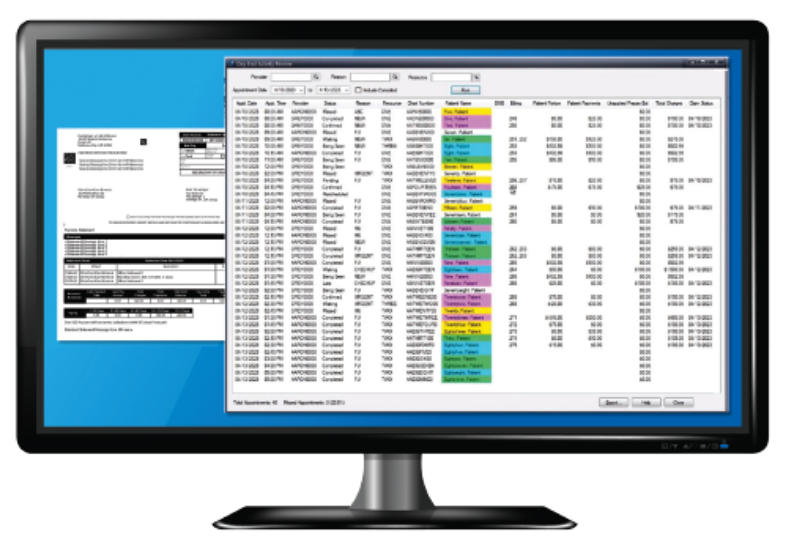
With CGM LYTEC 2026 medical billing software, you gain access to a robust practice management system designed to optimize your billing workflows. From patient intake to appointment setting, CGM LYTEC 2026 offers a comprehensive suite of tools to streamline every aspect of your billing operations.
- Enhanced medical billing: Simplify and expedite your billing process with features such as electronic claims submission, automated follow-up for outstanding payments, and insurance eligibility verification. CGM LYTEC 2026 medical billing software empowers you to take control of your practice’s financial health.
- Improved efficiency: The LYTEC medical billing software offers a user-friendly interface that streamlines daily tasks. Automate appointment reminders, manage patient demographics, and generate reports with ease.
- Increased productivity: The LYTEC mobile app allows you to access critical patient information and manage tasks remotely. This flexibility empowers both independent physicians and staff to be more productive from any location.
- Accurate diagnosis coding: Utilize a comprehensive database of diagnosis codes to ensure accurate and efficient claims processing.
- Streamlined patient accounting: Manage patient statements, track payments, and reduce administrative burdens with CGM LYTEC 2026’s robust patient accounting features.

Flexible, online patient appointments and scheduling
New to CGM LYTEC 2026, practices can offer online scheduling to meet rising patient expectations and help keep the daily schedule full.
With the flexible, online scheduling for CGM LYTEC, administrators can:
- Offer open slots by clinic
- Configure settings to control patient options, such as limiting a patient to scheduling a maximum number of appointments during a specified time period
- Designate days, times, providers, and available appointment types
- Automate scheduling or require administrative approval
- Allow patients to add themselves to the Wait List
Create a better patient journey with CGM LYTEC 2026. Leverage online appointment scheduling and offer a modern, patientfocused experience.

Convenient patient financing
New this year, you can offer patients a helpful financing option, powered by our eMEDIX clearinghouse and a seamless integration with CGM PAY.
With just a few clicks from your eMEDIX dashboard, you can connect patients to our third-party financing option, enabling them to manage out-of-pocket costs with a flexible payment plan. Patients enjoy greater access to care while your practice gets paid up front, reducing collection delays and administrative burdens.
The entire process is secure, efficient, and easy. Boost patient satisfaction and accelerate revenue velocity with help from CGM LYTEC and the eMEDIX clearinghouse.

Improved patient search
By popular demand, the patient search function has been expanded to allow users to search by a patient’s insurance ID. CGM LYTEC 2026 is smart enough to find a given patient even if the ID entered is actually the patient’s secondary or tertiary insurance.
Improved AR tracker
CGM LYTEC 2026 includes improvements to the AR tracker. Users can choose from saved AR filters, and now they can choose whether or not to automatically start with the filters they used during their previous session.

Easier online patient payments
With CGM LYTEC 2026, you can add a QR code to patient statements, making payments easier than ever. When patients scan the QR code, they’re instantly taken to a secure, mobile-friendly online payment page—no manual entry required.
This convenient feature, available in conjunction with our eMEDIX clearinghouse, streamlines the payment process, reduces barriers for patients, and helps your practice get paid faster

Electronic attachments for workers’ comp and auto claims
With CGM LYTEC 2026 and our eMEDIX clearinghouse, users can apply the familiar, electronic claim attachment workflow to workers’ comp and auto claims, making it easier to manage the overall claims process.

Upgrade to CGM LYTEC 2026.
Take advantage of these exciting new features, and see the host of other improvements we have made to better assist you in your revenue cycle operations.
CGM LYTEC is the power play of practice management software.
Ready to experience the CGM LYTEC 2026 difference?
Contact Dabbs Computer Consultants to learn more about the CGM LYTEC medical billing platform and how it can transform your practice. We offer expert advice and support to help you get the most out of your practice management system.